|
How the Normal Hip works
The hip is one of the body's largest joints. It is a ball-and-socket joint. The socket is formed by the acetabulum, which is part of the large pelvis bone. The ball is the femoral head, which is the upper end of the femur (thighbone).
The bone surfaces of the ball and socket are covered with articular cartilage, a smooth tissue that cushions the ends of the bones and enables them to move easily.
A thin tissue called synovial membrane surrounds the hip joint. In a healthy hip, this membrane makes a small amount of fluid that lubricates the cartilage and eliminates almost all friction during hip movement.
Bands of tissue called ligaments (the hip capsule) connect the ball to the socket and provide stability to the joint.
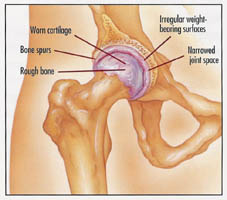
Common Causes of Hip Pain
The most common cause of chronic hip pain and disability is arthritis. Osteoarthritis, rheumatoid arthritis, and traumatic arthritis are the most common forms of this disease.
Hip Replacement
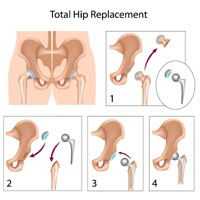
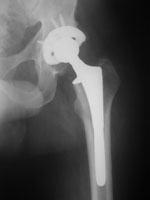
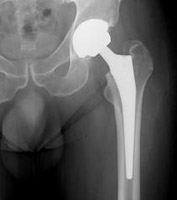
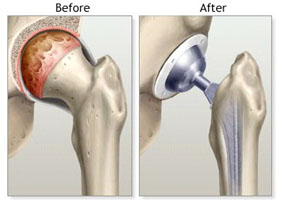
In a total hip replacement (also called total hip arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components.
• The damaged femoral head is removed and replaced with a metal stem that is placed into the hollow center of the femur. The femoral stem may be either cemented or "press fit" into the bone.
• A metal or ceramic ball is placed on the upper part of the stem. This ball replaces the damaged femoral head that was removed.
• The damaged cartilage surface of the socket (acetabulum) is removed and replaced with a metal socket. Screws or cement are sometimes used to hold the socket in place.
• A plastic, ceramic, or metal spacer is inserted between the new ball and the socket to allow for a smooth gliding surface.
Is Hip Replacement Surgery for You?
The decision to have hip replacement surgery should be a cooperative one made by you, your family and your orthopaedic surgeon.
Candidates for Surgery
There are no absolute age or weight restrictions for total hip replacements.
Recommendations for surgery are based on a patient's pain and disability, not age. Most patients who undergo total hip replacement are age 50 to 80, but orthopaedic surgeons evaluate patients individually. Total hip replacements have been performed successfully at all ages, from the young teenager with juvenile arthritis to the elderly patient with degenerative arthritis.
When Surgery Is Recommended
There are several reasons why your doctor may recommend hip replacement surgery. People who benefit from hip replacement surgery often have:
• Hip pain that limits everyday activities, such as walking or bending
• Hip pain that continues while resting, either day or night
• Stiffness in a hip that limits the ability to move or lift the leg
• Inadequate pain relief from anti-inflammatory drugs, physical therapy, or walking supports
Realistic Expectations of Patients
An important factor in deciding whether to have hip replacement surgery is understanding what the procedure can and cannot do. Most people who undergo hip replacement surgery experience a dramatic reduction of hip pain and a significant improvement in their ability to perform the common activities of daily living.
With normal use and activity, the material between the head and the socket of every hip replacement implant begins to wear. Excessive activity or being overweight may speed up this normal wear and cause the hip replacement to loosen and become painful. Therefore, most surgeons advise against high-impact activities such as running, jumping, or other high-impact sports.
Following total hip replacement Patient can do unlimited walking, swimming, driving, dancing, and other low-impact sports.
With appropriate activity modification, hip replacements can last for many years.
The Orthopaedic Assessment
An evaluation with an orthopaedic surgeon consists of several components.
• Medical history. Your orthopaedic surgeon will gather information about your general health and ask questions about the extent of your hip pain and how it affects your ability to perform everyday activities.
• Physical examination. This will assess hip mobility, strength, and alignment.
• X-rays. These images help to determine the extent of damage or deformity in your hip.
• Other tests. Occasionally other tests, such as a magnetic resonance imaging (MRI) scan, may be needed to determine the condition of the bone and soft tissues of your hip.
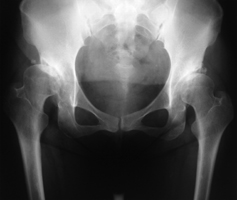
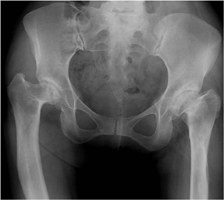
The Operation
You will most likely be admitted to the hospital on the day prior to surgery.
Anesthesia
After admission, you will be evaluated by a member of the anesthesia team. The most common types of anesthesia are general anesthesia (you are put to sleep) or spinal, epidural, or regional nerve block anesthesia (you are awake but your body is numb from the waist down). The anesthesia team, with your input, will determine which type of anesthesia will be best for you.
Implant Components
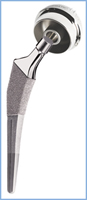
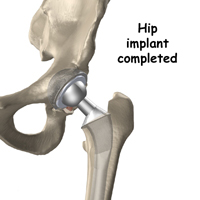
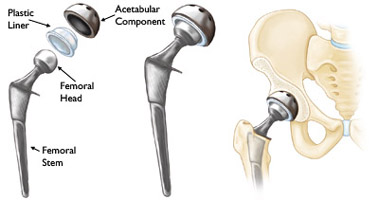
Many different types of designs and materials are currently used in artificial hip joints. All of them consist of two basic components: the ball component (made of highly polished strong metal or ceramic material) and the socket component (a durable cup of plastic, ceramic or metal, which may have an outer metal shell).
The prosthetic components may be "press fit" into the bone to allow your bone to grow onto the components or they may be cemented into place. The decision to press fit or to cement the components is based on a number of factors, such as the quality and strength of your bone. A combination of a cemented stem and a non-cemented socket may also be used.
Your orthopaedic surgeon will choose the type of prosthesis that best meets your needs.
Procedure
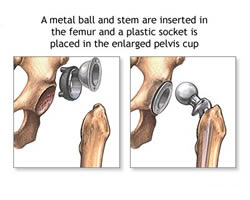
Your orthopaedic surgeon will remove the damaged cartilage and bone and then position new metal, plastic, or ceramic implants to restore the alignment and function of your hip.
After surgery, you will be moved to the recovery room where you will remain for several hours while your recovery from anesthesia is monitored. After you wake up, you will be taken to your hospital room.
Your Stay in the Hospital
You will most likely stay in the hospital for a few days.
Pain Management
After surgery, you will feel some pain, but your surgeon and nurses will provide medication to make you feel as comfortable as possible. Movement will begin soon after surgery, and when you feel less pain.
Physical Therapy
Walking and light activity are important to your recovery and will begin day after your surgery. Most patients who undergo total hip replacement begin standing and walking with the help of a walking support and a physical therapist the day after surgery.
Recovery
The success of your surgery will depend in large measure on how well you follow your orthopaedic surgeon's instructions regarding home care during the first few weeks after surgery.
Wound Care
The stitches or staples will be removed approximately 2 weeks after surgery.
Avoid getting the wound wet until it has thoroughly sealed and dried.
Diet
Some loss of appetite is common after surgery. A balanced diet, often with an iron supplement, is important to promote proper tissue healing and restore muscle strength. Drink plenty of fluids.
Activity
Exercise is a critical component of home care, particularly during the first few weeks after surgery. You should be able to resume most normal light activities of daily living within 3 to 6 weeks following surgery.
Your activity program should include:
• A graduated walking program to slowly increase your mobility.
• Resuming other normal household activities, such as sitting, standing, and climbing stairs
• Specific exercises to restore movement and strengthen your hip.
OUTCOMES
How Your New Hip Is Different
You may feel some numbness in the skin around your incision. You also may feel some stiffness, particularly with excessive bending. These differences often diminish with time, and most patients find these are minor compared with the pain and limited function they experienced prior to surgery.
Protecting Your Hip Replacement
There are many things you can do to protect your hip replacement and extend the life of your hip implant.
• Participate in a regular light exercise program to maintain proper strength and mobility of your new hip.
• Take special precautions to avoid falls and injuries
• See your orthopaedic surgeon periodically for routine follow-up examinations, even if your hip replacement seems to be doing fine.
|